..
Your doctor has decided that you need a test called Endoscopic Retrograde Cholangiopancreatography, or ERCP for short. This test is designed to image and treat disorders of the liver, bile ducts, and pancreas.
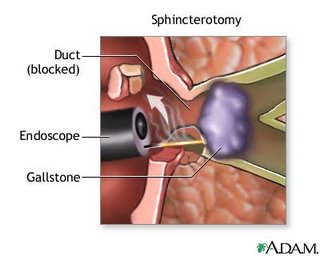 In many cases, a problem found during ERCP can be treated at the same time, thus avoiding major surgery. The procedure is usually performed by a Gastroenterologist, a doctor with special training in this field. The procedure might be a sphincterotomy, a removal of a stone, or a stent placement in order to keep a duct open.
In many cases, a problem found during ERCP can be treated at the same time, thus avoiding major surgery. The procedure is usually performed by a Gastroenterologist, a doctor with special training in this field. The procedure might be a sphincterotomy, a removal of a stone, or a stent placement in order to keep a duct open...
How Your Liver, gallbladder, and pancreas Work
To better understand ERCP, it is important that you understand a little about how the liver, gallbladder, and pancreas work. Your liver makes a substance called bile, a bitter yellowish-green fluid which helps digest your food. A duct is a hollow tube that carries fluid from one place to another, like a water pipe in your home. Bile is collected from the liver by a series of ducts that resemble branches of a tree. These branches come together at the main "trunk" called the common bile duct which drains into the intestine. Between meals about a quarter cup of bile is stored and concentrated in a side branch of the common bile duct called the gallbladder, a small pear-shaped hollow sac nestled beneath the liver in the right upper abdomen. The pancreas usually shares a common drain with the liver via its pancreatic duct. With each meal, bile enters the small intestine where it breaks up large globs of fat into smaller globs, a first step in digestion.
 A healthy gallbladder keeps bile flow moving like a mountain stream. However, when the gallbladder becomes diseased, the flow slows and the river turns into a swamp. The stagnant bile gradually crystallizes and the crystals clump together to form stones - like snowflakes making a snowball. (This is a totally separate disease from kidney stones that form in the urinary system. Having one kind of stone does not increase your risk of developing the other.)
A healthy gallbladder keeps bile flow moving like a mountain stream. However, when the gallbladder becomes diseased, the flow slows and the river turns into a swamp. The stagnant bile gradually crystallizes and the crystals clump together to form stones - like snowflakes making a snowball. (This is a totally separate disease from kidney stones that form in the urinary system. Having one kind of stone does not increase your risk of developing the other.)..
 Sometimes, a stone, scar tissue, or a tumor can block the ducts which drain the liver and/or pancreas. This is often an indication for ERCP which allows the most accurate means of visualizing the ducts and evaluating the problem.
Sometimes, a stone, scar tissue, or a tumor can block the ducts which drain the liver and/or pancreas. This is often an indication for ERCP which allows the most accurate means of visualizing the ducts and evaluating the problem...
How is ERCP performed?
 ERCP is performed in the X-ray department. There is very little preparation except fasting. After IV sedation with medications to make you sleepy and very relaxed, a small, thin tube with a videocamera (endoscope) is passed through the mouth. It is carefully guided down the foodpipe, past the stomach, and into the first part of the small intestine - called the duodenum.
ERCP is performed in the X-ray department. There is very little preparation except fasting. After IV sedation with medications to make you sleepy and very relaxed, a small, thin tube with a videocamera (endoscope) is passed through the mouth. It is carefully guided down the foodpipe, past the stomach, and into the first part of the small intestine - called the duodenum...
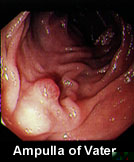 Using the special ERCP videoscope, your doctor can locate the small nipple-like opening called the ampulla which serves as the "drain" for your liver and pancreas.
Using the special ERCP videoscope, your doctor can locate the small nipple-like opening called the ampulla which serves as the "drain" for your liver and pancreas.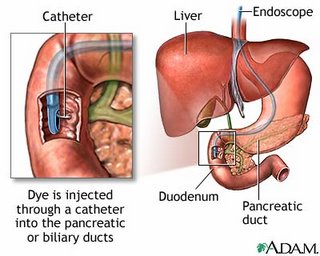 A small catheter is then placed through this opening and dye is carefully injected so that X-rays can be taken. If a problem is identified during ERCP, treatment can often be undertaken at the same time. Stones in the bile duct can be removed, narrow strictures can be dilated, and tumors can be biopsied and bypassed with a stent to relieve obstruction. The test takes 30 to 90 minutes to perform and is usually painless to the patient who is sedated.
A small catheter is then placed through this opening and dye is carefully injected so that X-rays can be taken. If a problem is identified during ERCP, treatment can often be undertaken at the same time. Stones in the bile duct can be removed, narrow strictures can be dilated, and tumors can be biopsied and bypassed with a stent to relieve obstruction. The test takes 30 to 90 minutes to perform and is usually painless to the patient who is sedated...
What Are The Risks of ERCP?
No test is 100% safe or without risk. Fortunately, ERCP can be performed in most patients without serious complications. On average, less than 10% of patients have complications from ERCP. The death rate is about 1 in 250, but these are usually sick hospitalized patients with multiple medical problems. The potential problems can be broken down into those related to the sedation, the scope procedure itself, and those specific to ERCP. Sedation risks To make the test comfortable, you will be given IV medications that make you sleepy. If you become too sleepy, it could suppress your breathing which could result in respiratory arrest. However, by monitoring your heart, blood oxygen level, and breathing closely, this can be prevented and this complication is rare.
..
Scope Risks
The thin, flexible videoscope is passed carefully and is usually well tolerated. However, in rare cases, damage to the lining of the upper digestive system can occur. This could cause bleeding or a hole in the intestinal wall. These complications might require surgery. Such damage occurs in less than 1 per 2000 cases. Another risk is choking on stomach contents during scope insertion. That is why it is so important not to eat or drink for the 8 hours before your examination.
..
ERCP Specific Risks
This test has some specific complications associated with injecting and instrumentation of the pancreatic duct. The most frequent complication by far is that of pancreatitis. In about 3 to 5% of cases, the pancreas gland becomes inflamed after ERCP and releases potent digestive juices directly into the surrounding tissue causing pancreatitis. Symptoms of pancreatitis include abdominal and back pain, nausea, and vomiting. In most cases, this complication gets better within 48 hours, but can be more severe in less than 1% of cases. This could result in a prolonged hospitalization, diabetes, fat malabsorption, and in rare cases, death. If the bile duct must be cut to relieve an obstruction or remove a stone, bleeding and perforation of the bowel may occur in 1 to 3% of cases. Failed ERCPIn some cases, the anatomy of the opening can prevent passage of the catheter into the ducts. Sometimes this is due to an intestinal pocket, or diverticulum, which distorts the normal anatomy. Failed ERCP occurs in about 3 to 5% of cases.
..
Preparing For ERCP
- Most ERCP exams are done in the morning. To prepare, you should not eat or drink anything after midnight the night before your test. If your ERCP is scheduled for the afternoon, you must remain totally fasting for at least 8 hours before your test.
- Be sure to tell your doctor about all allergies, especially those to shellfish, iodine, IVP dye, and X-ray contrast dye.
- Your regular medications can be taken with a sip of water on the morning of your exam - EXCEPT diabetic medications. If your are diabetic, your doctor will give you special instructions.
- You should be off all blood-thinning medications at least 3 days prior to your exam.
- If you have heart problems and have been told that you need antibiotics before procedures, alert your doctor.
- Please arrange for a driver to bring you home after the exam, preferably be a family member.
After ERCP
Usually the doctor will discuss the results right after the exam. Occasionally, an office visit will be arranged to discuss more complicated problems, or if you are too sleepy. If your test was done as an outpatient, you will usually be allowed to return home about two hours after your exam. This allows time for most of the sedation to wear off and to screen for complications. Plan to go straight home - not to a restaurant nor back to work. Summary ERCP is an excellent test to diagnose and treat disorders of the liver, bile ducts, and pancreas. It can prevent the need for major abdominal surgery and, most often, can be performed as an outpatient with minimal discomfort. Complications are most often mild and resolve quickly. If you have any questions or concerns about this test, discuss them with your doctor.
Percutaneous Transhepatic Cholangiography (PTC)
PTC is an invasive radiological procedure, where bile ducts are accessed from across the skin through the liver. Following administration of a local anesthetic, a needle is passed through the skin and into the liver, from where the bile duct is accessed. From here, contrast material, wires, and other special instruments can be placed into the bile duct. Complications include bleeding, formation of fistulas, and infections.
PTC it is often performed instead of an ERCP in situations were previous surgeries that displace the location of the major papilla relative to the stomach make ERCP impossible. These conditions include previous stomach resections and bowel surgeries with Billroth-II and Roux-en-Y anastomosis.
Like ERCP, PTC allows for diagnostic and therapeutic procedures such as tissue acquisition, stent placement, and dilation of strictures. Endoscopic sphincterotomy cannot be performed by the PTC method. However, PTC can sometimes be combined with ERCP to allow endoscopic sphincterotomy to be performed.
Unlike ERCP, PTC does not allow the pancreatic duct to be accessed or visualized.
..
To view information on another disease, click on Pancreatitis SOD Library.!
..

No comments:
Post a Comment